On this page... (hide)
- 1. Vision for the 3D Shape Sensing Needle
- 2. Background
- 3. Videos
- 4. What's New?
- 5. Links
1. Vision for the 3D Shape Sensing Needle
The manipulation of catheters, needles and similar minimally invasive devices to reach targets (such as tumors or other affected tissue) is the initial step of nearly all MRI-guided interventions. During breast or prostate biopsy procedures under MRI, the radiologist can mark the suspect tissue with surgical wires or extract tissue via the deployment of needles. In most cases, these long, slender needles deflect during insertion and manipulation in the body.
Consequently, many MR images need to be taken, in order to find the tip of the needle. It would be advantageous to know the position of the needle so that the image can be taken easily in only the plane of interest. Right now there is some guess and check work involved in the procedure: the patient is poked, the image is taken, the needle is moved and the patient is poked again, another image is taken, and the process repeats until the tip of the needle is found. A major need, in interventional therapy and diagnostic fields (especially in the prostate, breast and liver), is a method to anticipate needle deflections to allow for immediate compensation of a needle�s trajectory, and avoid increased risks to the patient.
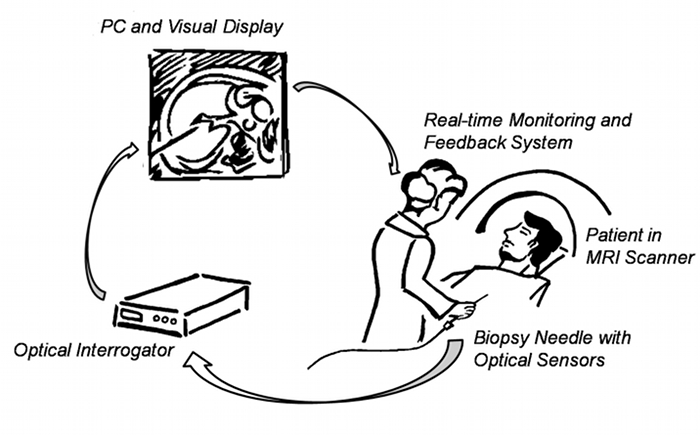
System overview of the biopsy needle with FBG sensors, used in a visual, physician controlled, feedback loop. Based on the needle�s deflections, MR images are autonomously updated in real-time and used by the physician to compensate for deviations.
2. Background
Current technologies for tracking devices include rapid MRI, MR-tracking and gradient based tracking (such as the Endoscout� by Robin Medical Inc). These methods are all limited not only because they require use of the MRI system during manipulation, but also because they are made of MRI-compatible metallic devices which can cause image distortions that lead to poor signal and/or inaccurate position information. Furthermore, the tracking methods require integration of electronics with the interventional devices, which increase device complexity and introduces the need for appropriate patient isolation electronics.
Recently, miniaturized fiber-optic sensors which incorporate fiber Bragg grating (FBG) technology have been developed for use in haptic (force and touch feedback) applications. The Bragg gratings in an optical fiber reflect a specific wavelength of light, corresponding to the spacing of the grating. As the fiber is strained, the spacing changes and the reflected wavelength shifts. Fiber optic Bragg grating (FBG) sensors can resolve small strains (on the order of 0.1 microstrain) and are immune to electromagnetic noise. Multiple sensors can be placed along a single fiber and multiplexed optically. FBG sensors have been demonstrated in prototype robotic fingers for NASA2 and appear to be an ideal technology for force and strain sensing (e.g., as a result of needle bending) in MRI interventions.
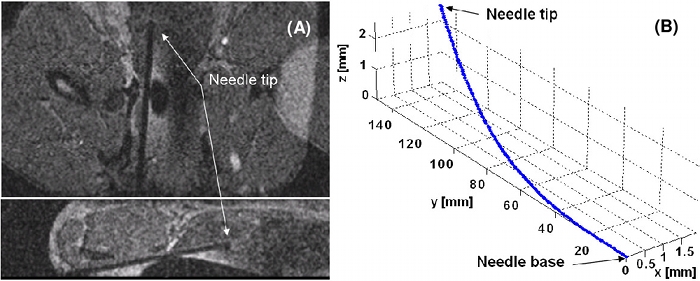
A. MRI of the prototype in the prostate of a mature male beagle. B. When this image was taken, the needle was deflected 2mm and 2.5mm in the x and z axes. (Scale exaggerated to highlight bending.)
3. Videos
http://www.youtube.com/watch?v=m1MR9QtOU4o
4. What's New?
- 15 Dec 2010 - Paper "Real-Time Estimation of 3-D Needle Shape and Deflection for MRI-Guided Interventions" published in IEEE/ASME Transactions in Mechatronics, in a focused section on Surgical and Interventional Medical Devices.
- 23-27 Aug 2010 - Attendance and poster "Real-time 3D shape determination of interventional tools and MRI scan plane control with miniature optical strain sensors,� presented at the North American Summer School in Surgical Robotics and Simulation in Seattle, WA
- 24 May 2010 - Poster presented at the 1st Bio Mechanical Engineering Conference at Stanford (BMECS) in Stanford, CA.
- 18-24 April 2009 - Oral presentation, �MRI-compatible Haptics: Strain sensing for real-time estimation of three dimensional needle deflection in MRI environments,� at the International Society for Magnetic Resonance in Medicine (ISMRM) 17th's Scientific Meeting and Exhibition.
- 12-16 Jan 2009 - Attendance and poster, �MRI-compatible Haptics: Strain sensing for real-time estimation of three dimensional needle deflection in MRI environments.�, presented at the Winter School on Medical Robotics and Computer-Integrated Interventional Systems in Baltimore, MD.
- 3-9 May 2008 - Oral presentation, �MRI-compatible Haptics: Feasibility of using optical fiber Bragg grating strain-sensors to detect deflection of needles in an MRI environment� at the International Society for Magnetic Resonance in Medicine (ISMRM) 16th's Scientific Meeting and Exhibition.
5. Links
Category: MedicalRobotics

